
Repairing Failing Dental Implants in Washington, DC
Implant placed by another dentist failing? Dr. Marlin specializes in salvaging compromised implants other offices cannot fix. Washington DC.
Repairing Failing Implants
Your Smile Deserves the Highest-Quality Implant Restoration
Are Dental Implants a Good Investment?
Rescue Failing Implants At a Top-Rated Implant Practice
Dental implants are one of the most significant advancements in dental technology due to their unsurpassed durability, versatility, and ability to restore natural function and aesthetics. With that said, dental implants and their respective restorations are prone to gum inflammation called peri-implant mucositis, which can progress to peri-implantitis and lead to dental implant failure.
Suppose you have failing dental implants in Washington, DC. In that case, you’re in excellent hands at Elite Prosthetic Dentistry because our prosthodontist has achieved virtually no bone loss in implants he placed 20 years ago! And his innovative, patented implant technology has been used successfully to restore more than 14,000 dental implants.
What Causes Failing Implants?
From one tooth to an entire arch or to stabilize dentures, implant dentistry offers a successful solution for many restorative problems. While dental implants are the most reliable and only permanent tooth replacement solution, any of the following factors can result in peri-implantitis and failing implants.
Poor oral hygiene and untreated gum disease can cause bacterial infection around implant sites, increasing the risk of peri-implantitis and implant failure. As such, gum disease must be resolved before implant surgery, and proper oral health must be maintained after your procedure.
Surgical errors, improper implant placement, not using surgical guides, or inadequate initial stability can lead to implant failure. Bone loss can also occur due to excessive mechanical load on the implant.
Over time, various factors, including tooth loss, gum disease, and certain health conditions, can cause bone to lose density and weaken. Integration with the underlying bone is essential for implants to provide stable, long-lasting support for a crown, bridge, or full mouth prosthesis. If the underlying bone is inadequate, a bone grafting procedure is required to ensure proper fusion with the jaw bone.
Implant surgery is a complex procedure that requires outstanding skills and precision. Expertise in implant surgery and restoration is key to implant longevity. Every mouth and set of dental implants is unique. Therefore, experience, proven expertise, and advanced technology are fundamental to achieving the best possible outcome.
It’s imperative to place an abutment and crown with the correct emergence profile (contour of the dental restoration where it meets the gum tissue). An over-contoured crown can make it difficult to clean, thereby increasing plaque growth/retention and the risk of gum inflammation.
Although the general health consequences of smoking are widely known, tobacco use increases the risk of several oral health issues. In terms of dental implants, research has shown a greater incidence of marginal bone loss, peri-implantitis, and implant failure, most notably in the grafted maxillary sinus area (upper back arch) in smokers.
Immune system disorders, steroid therapy, chemotherapy or radiosurgery in the neck area, and excessive bruxism (tooth clenching/grinding) can lead to dental implant failure. Although these issues don’t exclude candidacy, superb diagnostic and surgical skills are required to help ensure a successful outcome.
Dental Implant Patients
Peri-implant mucositis is a condition that leads to inflammation and infection of gum tissue surrounding dental implants. Early symptoms include swollen gums, tenderness, and oral sensitivity. As the condition progresses, possible repercussions include worsening jaw pain, gum recession, deepening gum pockets, exposure of implant threads, pus around implants, and loose posts.
Prompt peri-implantitis treatment in Washington, DC, from our experienced prosthodontist, can save implants by detoxifying and bone grafting them, sometimes without the need to remove the implant.
Preventing Implant Failures Requires Diagnostic and Surgical Expertise
At Elite Prosthetic Dentistry, we use cone-beam computed tomography (CBCT) to assess bone width, angulation, and density. This comprehensive and phased analysis is necessary to determine if your implant site requires a bone grafting procedure before implant placement. The 3D image created from the CBCT scan fabricates a precise surgical guide that provides exact positioning for your implants. After the fusion process, our in-house lab technician creates the ideal, natural emergence profile without interference from misplaced implants.
As a top-rated Washington, DC prosthodontist and implant surgeon, Dr. Gerald M. Marlin was an early adopter of CBCT technology in 2002, when it was introduced to the U.S. Since then, the technology has advanced from being merely preliminary viewing-analytic software to state-of-the-art, interactive software allowing virtual reality “placement” of implant images in ideal positions on the CBCT 3D radiographic image for presurgical planning. Over the last 15 years, Dr. Marlin has solely used CT-generated surgical guides, providing the most precise implant placement
The Proof Is
In Our Patients

Saving Failing Dental Implants
When you entrust ailing implants to our highly accomplished prosthodontist, treatment is based on your unique circumstances. As an example, one of our patients developed bone loss seven years after placement and restoration. To detoxify and re-graft the bone around a failing implant, the abutment and crown were removed, bone graft material was combined with a growth factor, and the implant was shielded under the protective gum tissue. Imaging after four months showed new bone formation that filled in around the side and top of the implant. After five months, the implant was exposed, and the abutment and crown were reseated, thereby saving the implant without the need to remove it!
Recognizing the Signs of Implant Trouble Early
Early recognition of implant problems dramatically improves the likelihood of successful treatment. Unfortunately, many patients do not seek evaluation until complications are advanced. Being aware of warning signs allows prompt intervention.
Bleeding or swollen gums around an implant are among the earliest signs of trouble. While some inflammation is normal immediately after placement, persistent inflammation beyond the first few weeks warrants evaluation. Increasing pocket depth (measured by probing around the implant) indicates advancing disease. Pus or drainage around the implant is a concerning sign of infection.
Some patients notice changes in implant mobility. A small amount of movement is normal immediately after placement and can occur when integration first occurs. But a tooth or implant that becomes progressively more mobile indicates compromised bone support and requires urgent evaluation.
Changes in bite or jaw position may indicate bone loss affecting implant support. Pain or discomfort around the implant, especially pain on biting, suggests a problem beneath the surface.
If you notice any of these signs, contact your dentist or Dr. Marlin immediately. Early evaluation and intervention often allow treatment that preserves the implant. Delayed diagnosis risks loss of the implant and additional bone loss that complicates replacement.
The Anatomy of Peri-Implantitis
To understand implant failure, one must understand peri-implantitis. Unlike tooth decay, which affects the tooth itself, peri-implantitis is an infection of the tissues and bone supporting the implant. It develops when bacteria colonize the space between the implant and the gum tissue, creating a pocket of infection similar to the periodontal pockets that develop around natural teeth with gum disease.
The infection extends progressively deeper, destroying gum tissue and bone around the implant. If untreated, the infection eventually undermines the implant’s support so completely that the implant becomes loose and fails.
What makes peri-implantitis particularly insidious is that it often develops without obvious symptoms until it is advanced. Unlike the acute pain of an abscessed natural tooth, peri-implantitis may cause no discomfort. A patient may not realize there is a problem until an implant becomes visibly loose or bleeding occurs.
This is why professional monitoring is so important. Even patients with excellent home care benefit from regular professional evaluation. Dr. Marlin’s examinations assess implant health, measure pocket depths, evaluate bone levels on radiographs, and identify early signs of trouble.
Risk Factors Beyond Surgical Technique
While surgical errors contribute to some implant failures, many failing implants resulted from proper surgery but developed problems afterward due to other factors. Understanding these risk factors helps patients understand what can be controlled and what requires vigilance.
Tobacco use is one of the most significant preventable risk factors. Smokers have significantly higher rates of implant failure and peri-implantitis. The mechanism is multiple: smoking impairs immune function, reduces blood supply to tissues, and promotes bacterial colonization. For smokers, implant success requires absolute commitment to excellent home care and more frequent professional monitoring.
Diabetes is another significant risk factor, particularly poorly controlled diabetes. Elevated blood glucose impairs immune function and bone healing. Diabetic patients benefit from more careful monitoring and sometimes more frequent professional cleanings.
Immune system disorders, including HIV infection and autoimmune conditions, affect implant success. Some medications, including certain steroids and chemotherapy agents, compromise healing and implant integration.
Bruxism (clenching and grinding) creates excessive mechanical forces on implants, potentially causing early bone loss. Patients with bruxism benefit from wearing a night guard to protect implants and natural teeth.
Oral hygiene is perhaps the most controllable risk factor. Patients who maintain meticulous home care and regular professional visits dramatically reduce peri-implantitis risk. This is why Dr. Marlin emphasizes that implant success is a partnership: he provides expert placement and monitoring, but patient commitment to care is equally important.
The Detoxification and Re-grafting Approach
When peri-implantitis is identified early, before severe bone loss has occurred, Dr. Marlin often recommends a salvage approach. Rather than immediately extracting the implant, he removes the crown and abutment to gain access to the implant surface.
The implant surface is then meticulously decontaminated. Specialized instruments remove the biofilm (bacterial coating) from the implant threads and surface. The goal is to eliminate the infection and create conditions for bone reattachment.
Once the implant is clean, bone graft material is placed around the defect. Often, this graft material is combined with a growth factor that stimulates new bone formation. The implant is then covered with gum tissue to shield it while bone heals and integrates.
Over months, new bone forms around the implant. Radiographic monitoring assesses bone fill and healing. Once adequate bone has reformed, the implant can be re-exposed and a new restoration fabricated.
This approach salvages implants that might otherwise have been lost. While it requires patience (several months of healing), it preserves the implant post (the most expensive and complex component) and often succeeds in stabilizing the implant for years of additional function.
When Extraction Is Necessary
Not all failing implants can be salvaged. Sometimes bone loss is too extensive, infection too advanced, or the implant itself mechanically compromised. In these situations, extraction is necessary to prevent further bone loss and infection.
Removing a failed implant requires care. The implant must be removed without further traumatizing adjacent bone or damaging surrounding teeth. This is why extraction of a failed implant is often best performed by an experienced prosthodontist rather than a general dentist.
Once the implant is removed, the socket is debrided and, if necessary, bone grafted to rebuild contours for future restoration. If the patient desires a replacement restoration, a period of healing and bone maturation is usually required before new implants can be placed or other restorative options pursued.
While implant loss is certainly disappointing, it is not catastrophic. Modern options for bone grafting and implant replacement are excellent. Many patients proceed successfully with replacement implants once healing is complete.
The Role of Emergence Profile in Prevention
One of the most overlooked factors in implant longevity is the emergence profile of the crown: the contour of the crown as it transitions from the tooth to the gum tissue. An ideal emergence profile is gradual and flowing, allowing the crown to be cleansed easily and gum tissue to sit comfortably around it.
A poorly contoured crown, one that is too bulky or projects excessively into the gum space, makes it difficult to clean the area. Food debris and bacteria accumulate in the space between the crown and gum. Over time, this leads to inflammation and infection.
Conversely, a crown that is too thin or undercontoured at the emergence profile may create inadequate gum support, leading to recession and exposure of the implant threads beneath.
Achieving ideal emergence profile requires meticulous attention during crown design and fabrication. Dr. Marlin’s prosthodontic training and his direct collaboration with his in-house laboratory ensure that every implant crown is designed and fabricated with proper emergence profile.
Long-Term Implant Health and Professional Partnerships
The implant failures Dr. Marlin treats are often the result of inadequate follow-up rather than poor initial placement. Patients who received implants from other offices may not have maintained regular professional contact. Without periodic evaluation, early signs of trouble go undetected until problems are advanced.
At Elite Prosthetic Dentistry, Dr. Marlin emphasizes ongoing partnership. After implants have been placed and crowns delivered, regular maintenance visits are essential. These visits allow assessment of implant health, measurement of pocket depths, radiographic evaluation of bone levels, and intervention at the earliest sign of trouble.
For patients who had implants placed elsewhere and are now experiencing problems, Dr. Marlin offers evaluation and rescue options. Many implants that other practitioners have given up on can be salvaged through expert assessment and targeted intervention.
The 3,900+ implants that Elite Prosthetic Dentistry has placed represent a commitment to excellence in every phase: surgical planning, placement technique, restoration design, and long-term maintenance. Patients who entrust their implant care to Dr. Marlin benefit not only from superior initial treatment but also from his dedication to protecting that investment through expert, ongoing care.
Your Implant Problems Have Solutions
If you have failing implants, damage around implants, or questions about existing implants, schedule a consultation with Dr. Gerald Marlin. With 40+ years of prosthodontic expertise and thousands of implant cases managed successfully, Dr. Marlin has encountered virtually every implant challenge and has the skills to address it.
Many implants that have been written off as unsalvageable can be treated successfully when evaluated by an experienced prosthodontist. Even implants that ultimately cannot be saved can be managed in ways that allow successful replacement or alternative restoration.
Your investment in implant therapy deserves expert, ongoing care. Whether your implants are stable and functioning excellently, or whether they require intervention and salvage, Dr. Marlin offers the expertise necessary to protect and optimize your long-term oral health.
Your Best Smile Is Within Reach
Schedule a consultation with Dr. Gerald Marlin to discuss your treatment options and take the first step toward a healthier, more confident smile.
Frequently Asked Questions
What are the signs of a failing dental implant?
Early warning signs include redness or swelling around the implant site, bleeding when brushing near the implant, discomfort or looseness of the implant crown, receding gum tissue around the implant, and a bad taste or odor near the implant. Recognizing these symptoms early dramatically improves the likelihood of successful treatment.
Can a failing dental implant be saved?
In many cases, yes. Dr. Marlin's patented implant technology has salvaged over 14,000 compromised implants. Treatment typically involves detoxification of the implant surface and re-grafting bone around the affected area. The earlier intervention begins, the better the outcome. In severe cases where the implant cannot be saved, it can be removed and replaced.
What causes dental implants to fail?
Common causes include poor oral hygiene leading to peri-implantitis, surgical errors during initial placement, inadequate bone support, over-contoured crowns that trap bacteria, smoking, immune disorders, certain medications, and bruxism (teeth grinding). Many failures Dr. Marlin treats were placed by other practitioners.
What is peri-implantitis and how is it treated?
Peri-implantitis is an inflammatory condition that attacks the bone and tissue surrounding a dental implant, similar to how gum disease affects natural teeth. It progresses from initial gum inflammation (peri-implant mucositis) to bone loss around the implant. Treatment involves detoxifying the implant surface, removing infected tissue, and bone grafting to rebuild lost support.
What is Dr. Marlin's success rate with dental implant repair?
Dr. Marlin maintains a 97% success rate with virtually no bone loss in implants placed 20 years ago. His patented implant technology and decades of specialized experience in implant salvage make Elite Prosthetic Dentistry a referral destination for patients with failing implants placed by other practitioners.
Related Case Studies
Explore similar cases demonstrating our expertise in advanced prosthetic dentistry.
 Complex
Complex Temporary Crowns Restore Patient's Smile in Just One Day with an Immediate Smile Makeover
Her dental implant looked artificial in her mouth and was impacting her smile. She had been very unhappy with her unsightly smile line and was beco...
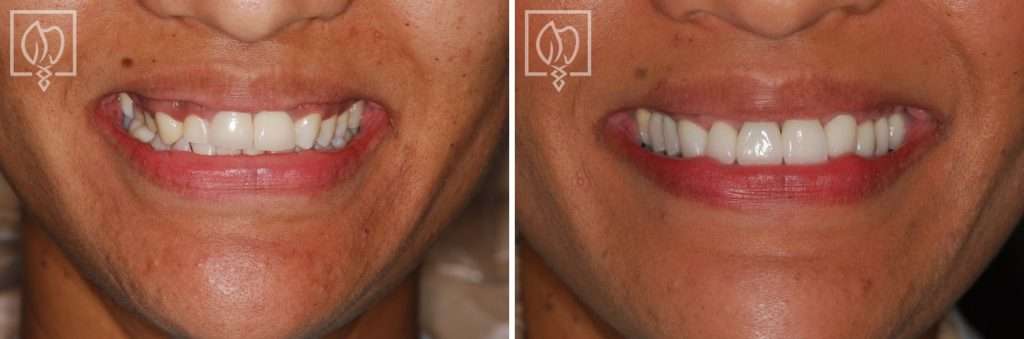 Complex
Complex Multi-Faceted Treatment for Patient Unhappy With Her Artificial-Looking Crowns, Teeth and Gums
Many patients come to Elite Prosthetic Dentistry unhappy with the appearance of their smile. A particular patient who sought our help was very unha...
 Standard
Standard Treating Kevin’s Collapsed Bite with a Complete Smile Makeover with New Dentures
Kevin came to us very dissatisfied with his existing condition. He looked much older than his age because his bite was collapsed and no one could r...
Related Articles
Deepen your knowledge with additional insights on this topic.
Rejuvenating a Ruined Implant Site Having Severely Damaged Bone
Even after a failed implant and significant bone loss, it is often possible to rebuild the ridge and restore a healthy foundation for a new implant.
If a Single Front Tooth is Replaced with an Implant, can it Look Natural?
A single front tooth implant can look completely natural with precision placement, custom abutments, and hand-crafted porcelain crowns. Washington, DC.
What is Precision Implant Placement (PIP)?
Learn what Precision Implant Placement (PIP) is and how meticulous planning ensures optimal implant positioning for long-lasting results in Washington, DC.
Ready to Transform Your Smile?
With 40+ years of experience and 3,900+ dental implants placed, Dr. Gerald Marlin delivers results that last. Schedule your consultation today.
