Learning the Lingo - Dental Implants
Understanding Dental Implant Terminology: A Comprehensive Guide
Dental implants are a safe and effective replacement for missing teeth. The implant is placed directly in your jawbone and integrates with your natural bone through a biological process that creates a permanent foundation for your new teeth. This implant then forms a stable, sturdy base for the artificial teeth that replace those you have lost. As you research implant treatment and consult with your prosthodontist, you will encounter various technical terms. Understanding this terminology helps you participate more actively in treatment planning and makes your consultation more productive.
What They Are: The Components of a Dental Implant
Understanding the different parts of a dental implant system is essential to grasping how the restoration works and how the different components fit together.
Implant: The implant itself is the foundational component of the entire restoration. It is a small rod, typically made of titanium or zirconia, that is surgically screwed directly into the jawbone. The implant acts as an artificial tooth root, replacing the root structure that was lost when your natural tooth was extracted. The implant remains below the gum line and is not visible after healing is complete.
The implant body has a threaded design that allows it to be screwed securely into the bone. This threaded design is critical because it increases the surface area in contact with bone, which enhances the strength of the biological bond that forms during osseointegration.
Abutment: The abutment is the connecting piece that bridges the gap between the implant and the crown. Abutments are custom-fabricated or selected from standardized options to fit the specific implant system being used. The abutment is attached to the top of the implant and extends above the gum line. The crown is then attached to the abutment.
The abutment’s design is critical to both the function and esthetics of the final restoration. A well-designed abutment allows the crown to be positioned at the proper angle and height, creating a natural-looking emergence profile where the crown emerges from the gum tissue.
Crown: The crown is the visible part of the tooth that you see in the mirror and that performs the function of chewing. It is a tooth-shaped cap that is attached to the abutment. The crown is typically custom-made to match the color, size, and shape of your adjacent natural teeth, creating a restoration that looks like a natural tooth.
The crown sits above the gum line and bears the forces of chewing. It must be precisely fabricated to create proper contact with opposing teeth and adjacent teeth, ensuring balanced forces during mastication.
What They’re Made Of: Materials in Implant Dentistry
The materials used in implant treatment have evolved significantly over the past three decades. Modern implant systems and restorations employ biocompatible materials that integrate successfully with bone and provide long-term durability.
Titanium: Most implants are typically made of titanium, a biocompatible metal that has been used in medical and dental implants for more than 40 years. Titanium is remarkably strong, resistant to corrosion, and highly biocompatible. The titanium implant surface is often treated to enhance osseointegration, the process by which bone bonds directly to the implant surface.
Titanium’s strength and biocompatibility make it the gold standard implant material. It can support heavy forces and typically remains stable for decades when properly placed and maintained.
Zirconia: Zirconia is an alternative implant material that is gaining popularity, particularly for patients who prefer metal-free restorations. Zirconia is a white ceramic material that is biocompatible, just like titanium. It is also very strong and has been used successfully in dental implants for more than 15 years.
Zirconia implants offer esthetic advantages, particularly for patients with thin gum tissues where metal shows through. However, the long-term success data for zirconia is not as extensive as for titanium. Both materials are excellent choices, and the specific material recommended depends on your individual situation.
Crown Materials: The crown attached to the implant is typically made of porcelain fused to metal (PFM), all-ceramic, or zirconia. These materials are tooth-colored and can be shaded to match adjacent natural teeth. The material chosen depends on the location of the implant, esthetic requirements, and functional demands.
Where They Go: Implant Positioning and Types
The location where an implant is placed in the jaw and the type of implant used influence long-term success and function.
Endosteal Implants: Placed directly in the jawbone, endosteal implants are typically shaped like small screws, cylinders, or plates, and they are by far the most commonly used type of implant. These implants are placed during a surgical procedure in which the bone is carefully prepared to receive the implant, and the implant is screwed securely into place.
Endosteal implants work well for patients who have adequate bone volume and bone quality. They are extremely successful when placed by experienced prosthodontic surgeons and properly restored.
Subperiosteal Implants: Placed under the gum tissue but on or above the jawbone, subperiosteal implants are mostly used for people with smaller jaws or shallow jawbones who do not have adequate bone volume for traditional endosteal implants. These implants are less commonly used in modern practice because bone augmentation procedures often allow for endosteal implant placement instead.
What Happens To Them: Biological and Clinical Processes
Once an implant is placed, several important biological and clinical processes determine whether it will achieve long-term success.
Osseointegration: This is perhaps the most critical concept in implant success. Osseointegration creates strength and durability by allowing bone to fuse directly to the implant surface in a biocompatible manner. Bone cells attach themselves directly to the titanium or zirconia surface, essentially locking the implant into the jawbone.
This biological integration typically requires three to six months. During this time, the implant must be protected from chewing forces to allow bone healing. Once osseointegration is complete, the implant becomes an integral part of your skeleton and can support considerable forces.
Osseointegrated implants can then support prosthetic tooth replacements of various designs and functionality. Anything from a single crown replacing one tooth to implant-retained dentures replacing all teeth in the upper and lower jaws can be fabricated. The teeth or crowns are usually made to match the enamel color of existing teeth to create a natural appearance.
Bone Augmentation: Not all patients have enough healthy bone to support dental implants. When bone volume is insufficient, it must be built up before implant placement through a process called bone augmentation. Procedures can include bone grafting, in which bone material is added to the jaw to increase volume and strength.
Bone grafting can utilize your own bone, harvested from another area of your body or from your jaw, or bone from other sources. Successful bone augmentation procedures have high success rates and can allow patients with significant bone loss to become candidates for dental implants.
Your Partnership in Implant Success
At Elite Prosthetic Dentistry in Washington DC and Bethesda, we specialize in dental implant treatment. Dr. Gerald Marlin, with over 40 years of experience and more than 3,900 implants placed, can help you understand these terms in the context of your specific situation and determine whether dental implants are the right solution for your missing teeth.
Understanding the terminology of implant dentistry empowers you to have more informed conversations with your dental team and to better understand the recommendations made for your treatment. If you have questions about dental implants and whether they might benefit you, we invite you to contact us today at Prosthetic Dentistry of Washington D.C. to discuss your options with an implant specialist.
Related Case Studies
Explore similar cases demonstrating our expertise in advanced prosthetic dentistry.
 Complex
Complex Temporary Crowns Restore Patient's Smile in Just One Day with an Immediate Smile Makeover
Her dental implant looked artificial in her mouth and was impacting her smile. She had been very unhappy with her unsightly smile line and was beco...
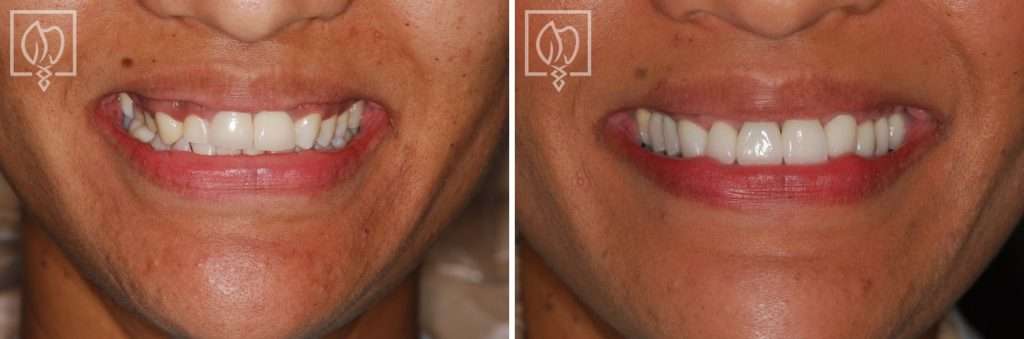 Complex
Complex Multi-Faceted Treatment for Patient Unhappy With Her Artificial-Looking Crowns, Teeth and Gums
Many patients come to Elite Prosthetic Dentistry unhappy with the appearance of their smile. A particular patient who sought our help was very unha...
 Standard
Standard Treating Kevin’s Collapsed Bite with a Complete Smile Makeover with New Dentures
Kevin came to us very dissatisfied with his existing condition. He looked much older than his age because his bite was collapsed and no one could r...
Related Articles
Deepen your knowledge with additional insights on this topic.
How is the Gummy Smile Fixed?
Dr. Marlin reshapes gum tissue and fabricates custom crowns to correct gummy smiles, creating a balanced and confident smile in Washington, DC.
Will Shifting Teeth Needing Splinting Look Individual? | Dr. Gerald Marlin
Splinted crowns stabilize shifting teeth while maintaining the appearance of individual natural teeth. Case study from Washington, DC prosthodontist.
Did Zoom Meetings Make You Unhappy with Your Smile?
Video calls made many people more aware of their smile. Explore cosmetic dentistry options to transform your confidence in Washington, DC.
